It’s summertime and the living is easy, fish are jumping and people are travelling, Including me! I specifically want to share my most recent travel experience by air.
My stress levels ramp up a couple of notches at the thoughts of traveling through airports. Airports equal airport security and as a person with diabetes I have a lot of organising to do to make this go as smoothly as possible.
I’ve travelled quite a bit but there is always something unexpected about it and I’ve just realised that I don’t travel very often by myself. I mostly travel with my well-travelled husband and two children and that is a very different experience - divide and conquer and all that.
Last weekend, I travelled to Amsterdam to attend the DxAmsterdam bloggers event sponsored by Abbott (more on that next week - it was great though and I learned lots). I had a couple of short flights, I travelled very light and no checked bags.
I thought I had covered everything; toiletries and cosmetics were in a clear plastic bag, medicines in another clear plastic bag, laptop easy to remove, no liquids… Or so I thought. Big, big sigh!
The first short flight was easier than expected, and boy did I savour this experience. In my home airport, I declared my medical devices and walked through the metal detector. IT DIDN’T BEEP!!!! So I could keep on walking. I didn’t have to volunteer for the pat down. I didn’t have to explain that I couldn’t go through any body scanner or why some pumps can and some don’t. I got to feel like a normal traveling person!!!
I did however make up for that seamless experience in my connecting airport where I had to do security all over again because I had to change terminals. I had to do the explaining, the intimate pat down, I had forgotten to take my camera and my glucagon out of both of my bags, so they had to be searched. I had a yogurt for my breakfast which was considered fluids and over the 100ml size, so that was confiscated but at least I had other food. So, so much to think about with diabetes and airport security.
The return trip was a bit smoother but still stressful. This time the trip to the airport was with friends; all who had diabetes:-) There were about seven of us going through security together. We all got held up for a variety of different reasons but not significantly.
I approached the body scanner and told the security agent I didn’t want to go through it. She was so nice and said that it was my choice and she didn’t mind which choice I made, at all. They did not have traditional metal detectors, so I was given the pat down search but I wasn’t taken away to a private area and it wasn’t overly intimate. I knew my bags would get flagged because they were packed very tight and the x ray machines have trouble seeing through overlaid items. But the agent had a quick look though and everything was fine. Onwards! All seven of us met up after security and it seemed we all had similar experiences and we all have similar anxiety and stress levels about it.
The next airport I did solo. Again, I had to go through airport security on my connection as I was changing terminals. This time I was ready for them. I removed a couple of additional items from my bag into a separate tray to make it easier to see through on the x ray. It did the trick. My bags went through and didn’t need to be search. This airport had both a body scanner and a metal detector so when I was directed towards the body scanner I said that I couldn’t go through it because of my CGM. I could go through the metal detector though.
This airports procedure is to call in the manager when someone opts out of the body scanner and I had to wait until he became availible. I had a very long layover so at least I didn’t have that stress.
When the manager arrived, I explained again why I was opting out and he asked if I would agree to a search. Sure! Then, he had to find two female agents to perform the pat down and swab of my pump and CGM. At this point, my bags had been abandoned at the end of the x ray machine so another agent was trying to reunite them with their owner. I could see them and him and identified myself, and the manager asked if the agent would gather them up and keep them behind the desk until we were done. I have to say even though this airport gave me the full works both times I went through the agents could not have been nicer about it. They were all so lovely!
The pat down was uneventful and I thanked everyone for being so nice and not making the experience any worse than it already was. I was almost home and I let the stress go.

My next flight is in July when I’m flying to the US with my family. Here are a couple of things that I will be doing for that trip;
Insulin Storage - when I travel to the US and I’m going for a couple of weeks I bring a flask. Yes, a thermos. And use reusable ice cubes. It works and it works brilliant! The ice cube are still a little bit frozen 24 hours later, which is usually when I get to my final destination.
[huge_it_gallery id="7"]
I get a new Doctor's Letter every couple of years.
You never know when you are going to need this or if ever. I never needed the doctor's letter until I started travelling with an insulin pump but I always had it. It pays to have it. I always make sure that my letter clearly states what devices should NOT go through what. I have been questioned a couple of times and on this occasion I was clear that I knew that the manufacturer states that my insulin pump cannot go through x-ray and that my CGM cannot go through any body imaging scanners because of the transmitter and that this instruction comes from the manufacturer.
I always bring some extra supplies.
One plus half times of supplies. Some sites recommend that you bring double of what you need but this takes up so much space. I definitely bring twice as much insulin because I once had it spoil in the heat. But the rest I just bring maybe a couple of days extra supplies.
Airport Security - Try not to stress too much about this. Know your rights, stay calm and polite (this can be a huge challenge), if you run into one of those people who makes you not want to be polite ask for that person’s manager.
This information isn’t really useful to anyone but I just thought it was considerate and worth mentioning;
We usually fly with United Airlines AND they have Nutritional information on their meals!!!!
On my last trip to the US I came across Sharps boxes in the bathroom of Newark Airport!!! How cool is that?
There is loads of information on really good diabetes websites and here are a couple I found really useful;
Diabetes UK Travel Tips
Good Blood Glucose Management on Long Trips from Insulin Nation
Medtronic Travel Information
Animas Travel information
Diabetes Ireland Travel Tips
https://www.diabetes.ie/living-with-diabetes/living-type-1/managing-diabetes/travelling/




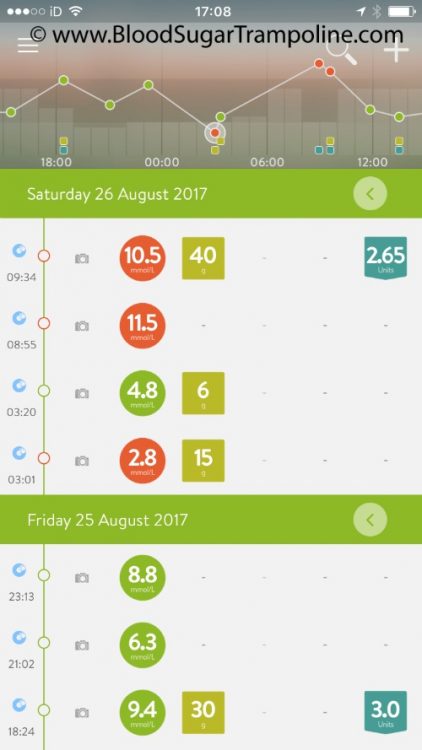
 Before breakfast, I checked my levels again; they were in target, so I took my insulin for my regular weekend breakfast of tea and toast also known as 40g of carbs and then ate it.
Before breakfast, I checked my levels again; they were in target, so I took my insulin for my regular weekend breakfast of tea and toast also known as 40g of carbs and then ate it.